Dr. Pattnaik's Laser Eye Institute New Delhi
Opening Hours : Monday to Saturday - 8am to 7pm
Contact : +91-8130780790 / 011-43444300

Winter can be a tough season for our eyes, with the season’s cold, dry temperatures, heavy winds, and harmful UV rays reflecting off snow and ice. Eyes require moisture, but during wintertime, there’s little to be found. Outdoors, there’s less humidity, and indoors, we dry up our homes blasting the heater. We don’t hate winter, but that doesn’t stop us from all-out crying after two minutes in the cold. Is it Abnormal? Nope—it’s our eyes’ normal biological response.
Your eyes need to stay lubricated to see, which doesn’t go well with cold, dry winter air. The wind and lack of moisture leads your eyes to tear up, trying to keep themselves at max visibility and minimum discomfort. It’s basically a reflex response—and when the tears overwhelm your tear ducts, they make a dramatic exit down your cheeks (and nose, so no worries about wiping it on a sleeve).
The lack of humidity makes your eyes tear more, as does brightness: All that light reflecting off snow makes your eyes more sensitive.
Glasses are your best defence against weeping on the way to work, because the glass creates a tiny greenhouse effect and keeps the air in front of your eyes more humid. Any glasses will work, but sunglasses pull double-duty against brightness.
If your eyes are still watering, try putting in a few wetting eyedrops before going outside. It may seem counterintuitive—add moisture to stop moisture—but the drops will keep your eyes from going into overdrive. Everyone’s eye sensitivity is genetically different, but if you’re facing excessive wetness and tearing up indoors, check with your doctor to make sure nothing else is up (could be a blocked duct, could be an abnormally small drainage system, or could be nothing).
Tearing is just your eyes’ response to dry winter air, and while it might be annoying to constantly explain that no, you’re not crying, it’s better than living with blurred vision or irritated peepers. Like most things, it comes down to genetics—and also like most things, sunglasses (and eyedrops) will help keep you cool.

Choosing Eye glasses for kids is sometimes a big challenge for parents sometimes, especially in first time users. Here are some tips. Most children who need eyeglasses are either near sighted or farsighted. Depending on the degree of visual correction necessary, your ophthalmologist will prescribe glasses for full- or part-time wear.
Here are some tips to ensure the right eye glasses for kids
o Avoid frames that will not please your childs’ personality and make him look uncool.
o Plastic frames are a better choice for children because they are more durable, less likely to be bent or broken, lighter in weight and less expensive.
o Each frame must be tried to make sure it fits the bridge. If any gaps exist between the bridge of the frame and the nose, the weight of the lenses will cause the glasses to slide, no matter how well the frame fits before the lenses are made. It is important that the glasses stay in place, because kids tend to look right over the top instead of the center of glasses.
o Temple that wraps all the way around the back of the ear help keep glasses from sliding down or dropping off a child’s face completely. You can try head band or ear loops for proper fit.
o Kids are not always careful when they put on and take off glasses, and spring hinges can help prevent the need for frequent adjustments and costly repairs. Spring hinges allow the temples to flex outward, away from the frames, without causing any damage.
o Lenses should be made of polycarbonate as they are lightweight and more impact-resistant. Also you can get thinner lenses if your child has high power glasses by choosing the right refractive index, which your optician can guide you the best.
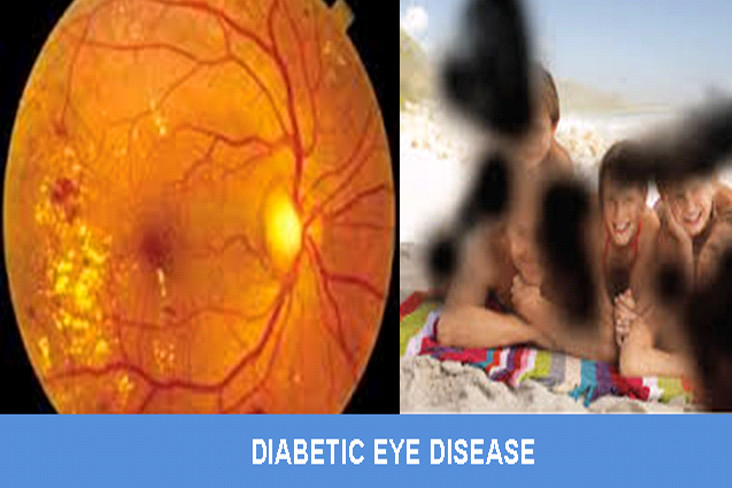
WHAT IS DIABETIC EYE DISEASE?
Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss or even blindness.
Diabetic eye disease may include:
WHAT IS DIABETIC RETINOPATHY?
Diabetic retinopathy is the most common diabetic eye disease and a leading cause of blindness in adults. It is caused by changes in the blood vessels of the retina.
In some people with diabetic retinopathy, blood vessels may swell and leak fluid. In other people, abnormal new blood vessels grow on the surface of the retina. The retina is the light-sensitive tissue at the back of the eye. A healthy retina is necessary for good vision.
If you have diabetic retinopathy, at first you may not notice changes to your vision. But over time, diabetic retinopathy can get worse and cause vision loss. Diabetic retinopathy usually affects both eyes.
WHAT ARE THE STAGES OF DIABETIC RETINOPATHY?
Diabetic retinopathy has four stages:
HOW DOES DIABETIC RETINOPATHY CAUSE VISION LOSS?
Blood vessels damaged from diabetic retinopathy can cause vision loss in two ways:
WHO IS AT RISK FOR DIABETIC RETINOPATHY?
All people with diabetes–both type 1 and type 2–are at risk. That’s why everyone with diabetes should get a comprehensive dilated eye exam at least once a year. The longer someone has diabetes, the more likely he or she will get diabetic retinopathy. Between 40 to 45 percent of Americans diagnosed with diabetes have some stage of diabetic retinopathy. If you have diabetic retinopathy, your doctor can recommend treatment to help prevent its progression.
During pregnancy, diabetic retinopathy may be a problem for women with diabetes. To protect vision, every pregnant woman with diabetes should have a comprehensive dilated eye exam as soon as possible. Your doctor may recommend additional exams during your pregnancy.
WHAT CAN I DO TO PROTECT MY VISION?
If you have diabetes get a comprehensive dilated eye exam at least once a year and remember:
If you have diabetic retinopathy, you may need an eye exam more often. People with proliferative retinopathy can reduce their risk of blindness by 95 percent with timely treatment and appropriate follow-up care.
The Diabetes Control and Complications Trial (DCCT) showed that better control of blood sugar levels slows the onset and progression of retinopathy. The people with diabetes who kept their blood sugar levels as close to normal as possible also had much less kidney and nerve disease. Better control also reduces the need for sight-saving laser surgery.
This level of blood sugar control may not be best for everyone, including some elderly patients, children under age 13, or people with heart disease. Be sure to ask your doctor if such a control program is right for you.
Other studies have shown that controlling elevated blood pressure and cholesterol can reduce the risk of vision loss. Controlling these will help your overall health as well as help protect your vision.
SYMPTOMS AND DETECTION
Does diabetic retinopathy have any symptoms?
Often there are no symptoms in the early stages of the disease, nor is there any pain. Don’t wait for symptoms. Be sure to have a comprehensive dilated eye exam at least once a year.
Blurred vision may occur when the macula—the part of the retina that provides sharp central vision—swells from leaking fluid. This condition is called macular edema.
If new blood vessels grow on the surface of the retina, they can bleed into the eye and block vision.
What are the symptoms of proliferative retinopathy if bleeding occurs?
At first, you will see a few specks of blood, or spots, “floating” in your vision. If spots occur, see your eye care professional as soon as possible. You may need treatment before more serious bleeding occurs. Hemorrhages tend to happen more than once, often during sleep.
Sometimes, without treatment, the spots clear, and you will see better. However, bleeding can reoccur and cause severely blurred vision. You need to be examined by your eye care professional at the first sign of blurred vision, before more bleeding occurs.
If left untreated, proliferative retinopathy can cause severe vision loss and even blindness. Also, the earlier you receive treatment, the more likely treatment will be effective.
How are diabetic retinopathy and macular edema detected?
Diabetic retinopathy and macular edema are detected during a comprehensive eye exam that includes:
Your eye care professional checks your retina for early signs of the disease, including:
If your eye care professional believes you need treatment for macular edema, he or she may suggest a fluorescein angiogram and OCT Macula. In this Fluorescein angiogram, a special dye is injected into your arm. Pictures are taken as the dye passes through the blood vessels in your retina. The test allows your eye care professional to identify any leaking blood vessels and recommend treatment. OCT quantifies the amount of swelling in the macula and identifies the layers involved.

Lacrimation is the secretion of tears, which often serve to clean and lubricate the eyes in response to irritation of the eyes. Tears formed through crying are associated with strong internal emotions such as sorrow, awe and pleasure. Laughing and yawning also result in production of tears. They also contain enzymes that neutralize the microorganisms that colonize the eye. Tears are essential for good eye health.
DRY EYE SYNDROME
In dry eye syndrome, the eye doesn’t produce enough tears, or the tears have a chemical composition that causes them to evaporate too quickly. Dry eye syndrome is caused by a chronic lack of sufficient lubrication and moisture on the surface of the eye. Its consequences range from subtle and constant irritation to inflammation of the eye. If left untreated, this condition can lead to pain, ulcers, or scars on the cornea, and some loss of vision. However, permanent loss of vision from dry eye is uncommon.
Persistent dryness, scratchiness, red eyes and a burning sensation are common symptoms of dry eyes. These symptoms alone may prompt your eye doctor to diagnose dry eye syndrome.
Dry eyes can become red and irritated, causing a feeling of scratchiness.
But sometimes your eye doctor may want to measure the amount of tears in your eyes. A thin strip of filter paper placed under the lower eyelid, called a Schirmer test, is one way to measure tear production.
Another symptom of dry eyes is a “foreign body sensation,” which is a feeling that something is in your eye.
And it may seem odd, but dry eye syndrome also can cause watery eyes. This is because dryness on the eye’s surface sometimes will overstimulate production of the watery component of your tears as a protective mechanism.
CAUSES OF DRY EYE
Dry eye syndrome has several causes:
TREATMENT FOR DRY EYES
Dry eye syndrome is an ongoing condition that may not be completely and permanently cured (depends on the cause), but the accompanying dryness, scratchiness and burning can be managed.
Lorem ipsum dolor sit amet, consectetuer adipiscing elit, sed diam nonummy nibh euismod tincidunt ut laoreet dolore magna aliquam erat volutpat. Ut wisi enim ad minim veniam, quis nostrud exerci tation ullamcorper suscipit lobortis nisl ut aliquip ex ea commodo consequat.